Organ donation is a sensitive issue for many people to think about and discuss but it is the difference between life and death for a person waiting for a transplant.
Many diseases can cause severe damage to the lungs that cannot be repaired by medication or surgery. The only hope for restoring normal lung function in this instance may be a lung transplant. In Europe, there is a long-standing shortage of organ donors, while the number of people waiting for a lung transplant is expected to rise.
This factsheet explains what organ donation is, how it can benefit people and how you can register to become a donor.
What is organ donation?
 Organ donation is the removal of organs from the human body after a person has died. These are donated to people who have damaged organs that need replacing. Receiving an organ transplant can save their life, increase their life expectancy and significantly increase their quality of life.
Organ donation is the removal of organs from the human body after a person has died. These are donated to people who have damaged organs that need replacing. Receiving an organ transplant can save their life, increase their life expectancy and significantly increase their quality of life.
Every person has a free choice whether they want their organs to be donated after they pass away. It needs to be discussed with friends or family and it is best to think about this while you are in good health. In most European countries, you can register as an organ donor, but your relatives will still need to allow the donation to take place when you die.
There are no good or bad decisions in deciding to donate an organ; however, it is very import that your closest relatives are aware of your intentions as it will help them to agree or not agree with donating your lungs.
When can I become a donor?
The majority of organs are donated when a person has suffered a severe trauma that has severely damaged their brain and affected their ability to breathe. The heart is kept beating by artificial sources, but a person is unable to breathe for themselves.
In each country there are also strict legal criteria for when an organ can be donated. This takes into account how compatible organs are and considers factors such as sex, age and blood group of both the donor and the recipient. It is also important to remember that the identity of the donor will remain anonymous and not told to the person who receives an organ.
Lung transplants
If a person with severe lung disease has tried all other treatment options and their condition hasn’t improved, they may eligible for a lung transplant.
The transplantation team make sure that lungs are donated to people who will receive the maximum benefit from the donation and who will take care of this gift. For example, people who continue to smoke are not eligible for lung transplantation. The chances of lung transplant patients surviving at least three years in 2012 are between 65–75%.
A person on a lung transplant waiting list will be very ill and usually has a life expectancy of 18 months or less. Their quality of life is likely to be significantly reduced. Their lungs will be badly damaged and they may require oxygen 24 hours a day to keep them breathing, or need a wheelchair to get around. They may receive a single or double lung transplant, or both a heart and lung transplant, depending on their condition.
This is the case for many lung conditions.
| Lung condition | Is lung transplant a possible treatment option? |
| Cystic fibrosis (CF) | In severe cases of CF, when the lungs stop working, a transplant is recommended. A double transplant is always required as the condition affects both lungs. These patients are typically aged 20–30 when they receive new lungs. |
| Chronic obstructive pulmonary disease (COPD) |
Lung transplantation is an option for only a small number of people with COPD, and only after other treatments (including pulmonary rehabilitation) have been tried. In most countries there is an upper age limit to qualify for a transplant as older people are less likely to survive. A more common operation is to remove a section of the lung that’s no longer working to give more space for the healthier lung to work. |
| Alpha 1-antitrypsin | People with the condition could require either a single or a double lung transplant. Some people will also develop chronic liver disease and may also require a liver transplant. As with all other conditions, it is only an option when all other treatment options have failed. |
| Interstitial lung diseases, such as pulmonary fibrosis or sarcoidosis |
People with severe, chronic cases of these rare diseases may be eligible for a lung transplant, but this is not a common treatment for this disease. |
| Lymphangioleiomyomatosis (LAM) |
Lung transplantation is a possibility for people with LAM, although this is only undertaken in severe cases. |
| Pulmonary hypertension | For people with severe pulmonary hypertension, a heart–lung transplant may be an option. As this involves transplanting both the healthy lungs and heart from a donor, there are minimal opportunities for it to be carried out. |
| Lung cancer | Lung transplantation is not an option for people who have developed lung cancer as the cancer is likely to return again in the new lungs. |
What are the benefits of a transplant?
Transplantation is the last option left to produce a major improvement in lung function and give someone a further chance at life. To understand the true benefits of a lung transplant, two lung transplant patients share their stories:
Case study: Justine Laymond
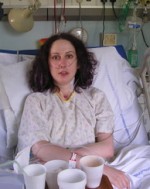 Justine suffers from a rare lung condition, known as lymphangioleiomyomatosis (LAM). It leads to a progressive decline in lung function and there is no known cure for the condition, which affects women usually of child-bearing age. Justine suffered 15 lung collapses, along with severe chest pain, over a number of years.
Justine suffers from a rare lung condition, known as lymphangioleiomyomatosis (LAM). It leads to a progressive decline in lung function and there is no known cure for the condition, which affects women usually of child-bearing age. Justine suffered 15 lung collapses, along with severe chest pain, over a number of years.
Gradually her lung function declined until she was hospitalised with only 30% lung capacity. She required oxygen all the time, and was wheelchair dependant. She was even put into a medically induced coma for a time. After three false alarms and 16 months in hospital, she was told that a pair of lungs had been donated and she could have a transplant.
 “I can’t even put into words how I felt at this moment. It was as if the whole room lit up. The thought that someone else had recently died was upsetting but this was an amazing, generous gift that they left behind them. I was out of hospital in 3 weeks and I no longer required oxygen or a wheelchair. As well as physical improvements in my condition, I was also mentally a different person. I now set myself a new goal each year. I’ve learned a range of new sports and took part in the European Transplant Games. I’ve also sailed around the world and visited countries which I could never have done before.
“I can’t even put into words how I felt at this moment. It was as if the whole room lit up. The thought that someone else had recently died was upsetting but this was an amazing, generous gift that they left behind them. I was out of hospital in 3 weeks and I no longer required oxygen or a wheelchair. As well as physical improvements in my condition, I was also mentally a different person. I now set myself a new goal each year. I’ve learned a range of new sports and took part in the European Transplant Games. I’ve also sailed around the world and visited countries which I could never have done before.
“I am so grateful for this gift and I now spend my life making sure I live it to the full. I would encourage more people to talk about organ donation and make sure others are aware of it. Most people would want to take this gift if they’d been in my position and I hope this would encourage them to also think about giving it.”
Case study: Kirstie Tancock
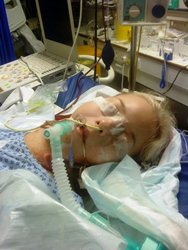 Kirstie was born with cystic fibrosis. Her lungs were so badly damaged from the condition, that by the age of 21, she needed a double lung transplant. Her illness became so bad that she was connected to an extracorporeal membrane oxygenation (ECMO) machine, which gave her the ventilation needed to keep her alive while she waited for the transplant.
Kirstie was born with cystic fibrosis. Her lungs were so badly damaged from the condition, that by the age of 21, she needed a double lung transplant. Her illness became so bad that she was connected to an extracorporeal membrane oxygenation (ECMO) machine, which gave her the ventilation needed to keep her alive while she waited for the transplant.
“Most of my life I was struggling for breath or I had a terrible cough and my lungs were full of mucus. Now, I can just breathe. I don’t have to think about it, it just happens. I feel free, like I’m the person I was always supposed to be and able to achieve things I never thought I could.
 “Everything has improved since my transplant. There is no medical regime for the length of the whole day. No machinery to take with you on a rare outing. I don’t have to worry that I haven’t got round to creating memory boxes and writing my funeral plan. I can run, I can sing, I can laugh, I can dance and I can live because I can breathe. If people are considering becoming an organ donor, I I would ask them if their daughter, sister, bother, mother, son, husband, wife, needed a life-saving transplant, would they want them to get it? If you’re willing to accept an organ you should be willing to give one.”
“Everything has improved since my transplant. There is no medical regime for the length of the whole day. No machinery to take with you on a rare outing. I don’t have to worry that I haven’t got round to creating memory boxes and writing my funeral plan. I can run, I can sing, I can laugh, I can dance and I can live because I can breathe. If people are considering becoming an organ donor, I I would ask them if their daughter, sister, bother, mother, son, husband, wife, needed a life-saving transplant, would they want them to get it? If you’re willing to accept an organ you should be willing to give one.”
People who receive transplants still have to take life-long medication for the rest of their lives to avoid infection and rejection of their new organ. They also have to make frequent visits to the hospital to check how their body has reacted to the new organ. In addition, these patients will take part in pulmonary rehabilitation programmes and are given advice on how to lead an active life to gain full the full benefit of the lungs they received.
However, this level of care is usually far less than a person needed prior to their transplant and they often see a significant improvement in their quality of life.
What are the risks of a transplant?
The main risk is that a person’s body could reject the new lung. This results in the immune system attacking the new tissue, as it believes it to be harmful. This can lead to a reduced lung function, which could happen quickly or slowly over time. There are many different drugs that can be taken to try to stop the immune system rejecting the organ.
How can I donate my lungs?
The process for organ donation differs from one country to another. In some European countries, such as Spain, Austria and Belgium, citizens are automatically considered to be a donor, although your family will still be consulted when you die. You also have an option to actively opt in, which means the family will just be made aware of your decision, or you can opt out if you do not wish your organs to be used.
In other countries, such as the UK, you must volunteer and opt in for your organs to be donated upon your death. It is important to know that a doctor, who hasn’t been directly treating you, will make the decision whether your organs are suitable for donation. This ensures that decisions about your treatment are never linked to the decision to donate or not donate your organs.
Check how the policy in your country operates to find out how you can donate your lungs. One useful website to start with is the Global Observatory on Donation and Transplantation:
What factors could prevent my organs being used?
There are a number of reasons your organs might not be suitable for donation, even if you have agreed to donate them.
Medical conditions: Only well-functioning organs can be used. If you have cancer, HIV or an infectious disease, your organs are unlikely to be used for a transplant.
Damage: In the case of death by injury, organs may be too badly damaged to be used.
Family consent: In some European countries in the event of death, families are consulted and must also give permission for organs to be used. Even if you have agreed to donate your organs, this decision could still be overturned by the family. It is therefore essential to discuss your wishes with your family and friends in advance so they are aware of your wishes.
Organ donation across countries
 Organ donation between European countries is a very complex issue. Some countries operate individually and do not allow organs donated in their country to be given to a patient in another country.
Organ donation between European countries is a very complex issue. Some countries operate individually and do not allow organs donated in their country to be given to a patient in another country.
Other countries, such as those in Scandanavia, belong to a network (in this case, the Scandiatransplant network), which allows the exchange or organs and tissue between participating transplant centres in five different countries. This is also the case for Austria, Belgium, Croatia, Germany, Luxembourg, the Netherlands and Slovenia, who belong to the Eurotransplant International Foundation.
EU action
The demand for organs outweighs supply all over the European territory. These shortages can generate organ trafficking, where criminals try to steal and traffic organs into other countries for money, which is strongly condemned by lung health and transplant societies across Europe.
To help combat this in 2008, the EU proposed an ‘Action plan on Organ Donation and Transplantation’ for 2009–2015.
One of the key priority areas in this plan was to improve the mobility of patients and donors as part of cooperation between member states. You can find out more about the current EU strategy on their website:
Further reading
The World Health Organization (WHO) has established a set of ‘Guiding Principles for Transplantation’. Visit the linka below to understand more about the ethical principles surrounding transplantation, proposed by the
WHO: www.who.int/transplantation.
