The respiratory system is the district with the highest incidence and prevalence of infections due to the obvious reason of its easy and wide access to foreign agents.
Rhinosinusitis is represented in most cases by viral infections of the common cold, only rarely contaminated by bacterial overlap. These are diseases with spontaneous resolution, usually without the need for antibiotic treatment, with the possible use of symptomatic treatments aimed at controlling fever and hypersecretion.
Rhinosinusitis can be a major pathological problem when accompanied by high hyperpyrexia, last for more than ten days, produce mucopurulent secretions or are associated with significant low respiratory symptoms. Such conditions open up the reasonable opportunity for antibiotic treatment.
Respiratory tract infection and inflammation
The diagnosis of acute bronchitis is usually clinical, therefore based on the objectivity of the patient, who manifests cough, fever, and has fairly typical auscultatory signs in the form of humid noises, crackles, any wheezing. The auscultatory finding is however very variable, it can also be silent even in the presence of a relevant infection, and depends on the degree of anatomical damage to the bronchial tree that has developed following previous recurrent infections.
 An X-ray examination is indicated in cases of suspected pneumonia, or in conditions of particular risk, for example in the elderly. In these circumstances, an examination of the sputum and a related antibiogram may also be appropriate.
An X-ray examination is indicated in cases of suspected pneumonia, or in conditions of particular risk, for example in the elderly. In these circumstances, an examination of the sputum and a related antibiogram may also be appropriate.
However, acute bronchitis tends to spontaneous self-resolution, favored by a supportive anti-inflammatory treatment as well as adequate hydration.
The boundary dividing the need or the uselessness of antibiotic treatment is often blurred. On the one hand, bronchitis represent a typical pathological area of antibiotic abuse; on the other hand, it would be deleterious to leave the infectious focus free to produce irreversible lesions to the bronchial tree for the sole obstinacy to avoid the use of antibiotics.
Therefore, the usual classification of pneumonia is not of an etiological but environmental type, recognizing community pneumonias (ie arising in the normal community of life) and nosocomial pneumonia, that is linked to hospitalization. The identification of a specific nosocomial category takes into account the epidemiological relevance of a complication that is often difficult to prevent or control, namely the superimposition of a respiratory infection in a patient hospitalized for other reasons.
Another way to classify pneumonia
– older but always practical for its clinical value – is that linked to anatomical localization and radiological findings. They therefore stand out
- lobar pneumonia, linked to the involvement of an entire lung lobe due to the spread of the infectious process by contiguity from the alveoli to neighboring areas, but without going beyond the serous
- lobular or broncholobular pneumonia, with multiple and disseminated thickening, including in both lungs
- interstitial pneumonia, with involvement of the connective, interlobar and interalveolar septa.
 Immunological diagnostics has expanded the possibilities of identifying the etiology of pneumonia, allowing to identify pathological antibody rates for various agents including Mycoplasma, Chlamydia, Legionella. The qualitative antibody profile distinguishes recent infection (increase in IgM) from a previous one (increase in IgG).
Immunological diagnostics has expanded the possibilities of identifying the etiology of pneumonia, allowing to identify pathological antibody rates for various agents including Mycoplasma, Chlamydia, Legionella. The qualitative antibody profile distinguishes recent infection (increase in IgM) from a previous one (increase in IgG).
The elevation of numerous inflammatory parameters, however non-specific, is usual: ESR, PCR, alpha2-globulins, neutrophilia.
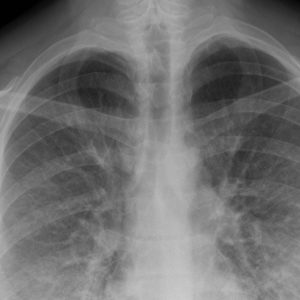
The radiological examination may show school-type images (frank lobar densities), but more often the display is in the form of multiple thickenings, spot, or ground glass (especially in interstitial forms).
